Autism and gastrointestinal problems go hand-in-hand for many kids. To demonstrate, a meta-analysis of several studies published by the Journal of Pediatrics estimates that “the odds of GI symptoms in children with ASD are four times more prevalent than for children without ASD.” Moreover, the analysis indicated higher levels of GI symptoms in all four areas, including general GI concerns, diarrhea, constipation, and abdominal pain.
In this article, we will discuss constipation and diarrhea, including:
- Common signs of constipation in autism
- Possible causes of chronic constipation and/or diarrhea
- Lifestyle tips to help alleviate constipation and diarrhea
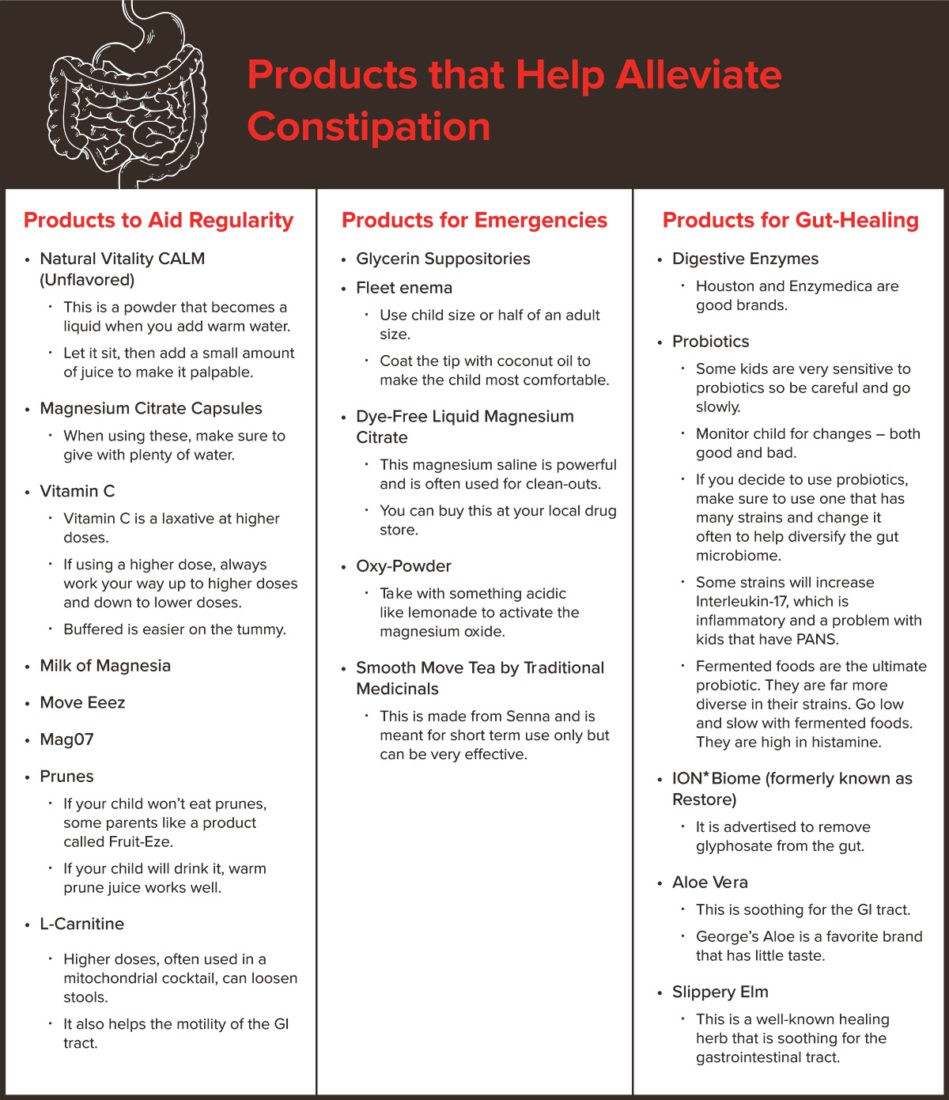
- Products that help alleviate constipation
- Warning about MiraLAX
If your child is still suffering despite dietary intervention, supplementation, and the remedies mentioned on this page, please read Complex Gastrointestinal Issues.
Constipation in Autism
When we think of constipation, we usually think of temporary episodes when our stool resembles hard, little rocks that are difficult to push out. This kind of constipation typically resolves with lifestyle changes such as adding more water, fruit, veggies, and fiber to your diet.
However, this usually isn’t the type of constipation children with autism deal with. The kind of constipation they deal with is chronic and very painful. Sometimes, intermittent bouts of diarrhea accompany it.
Can My Child Be Constipated Even Though They have Daily Bowel Movements?
Yes. In fact, many parents of kids with autism do not even know their child is constipated because the child has daily bowel movements. The child is simply not excreting enough stool.
At TACA conferences, doctors tell parents that you should see 8-10 inches of stool per day. If your child skips a day, then they have that much more stool to expel.
Therefore, it’s essential to pay attention to the following three things to know if your child’s bowel habits are healthy or not:
- The stool’s texture:
- It should be formed, yet soft and easy to pass
- Frequency of occurrence:
- Bowel movements should occur on a daily basis
- The amount of stool expelled:
- Doctors suggest 8-10 inches per day
Signs of Constipation In Autism
Because many children with autism struggle with communication and interoception (the ability to feel and understand what’s going on in our bodies), your child may not be able to verbally communicate to you that they are having trouble pooping or that their abdomen hurts. Consequently, parents often have to rely on behaviors and external clues to know if their child is suffering from constipation.
Below, you will find a list of common signs and symptoms that may indicate your child is constipated.
Troubled Sleep
A constipated child often wakes in the middle of the night because of discomfort and has difficulty getting back to sleep.
Aggression and Self-Injurious Behavior
Constipation is extremely painful. And, if your child can’t tell you that they’re in pain, their only option is to use their behavior as a form of communication. This misery is often expressed through self-injurious and aggressive behaviors. Tragically, many of our kids have been suffering from this pain for a very long time; therefore, they don’t know what it’s like to live without extreme gastrointestinal pain.
Loose Bowel Movements
Interestingly, loose stool can be a red flag for constipation. If large masses of stool harden and collect in the colon or rectum, they can form a blockage. When this occurs, soft or liquid stool squeezes around that blockage, resulting in frequent or involuntary loose bowel movements, which can be mistaken for diarrhea.
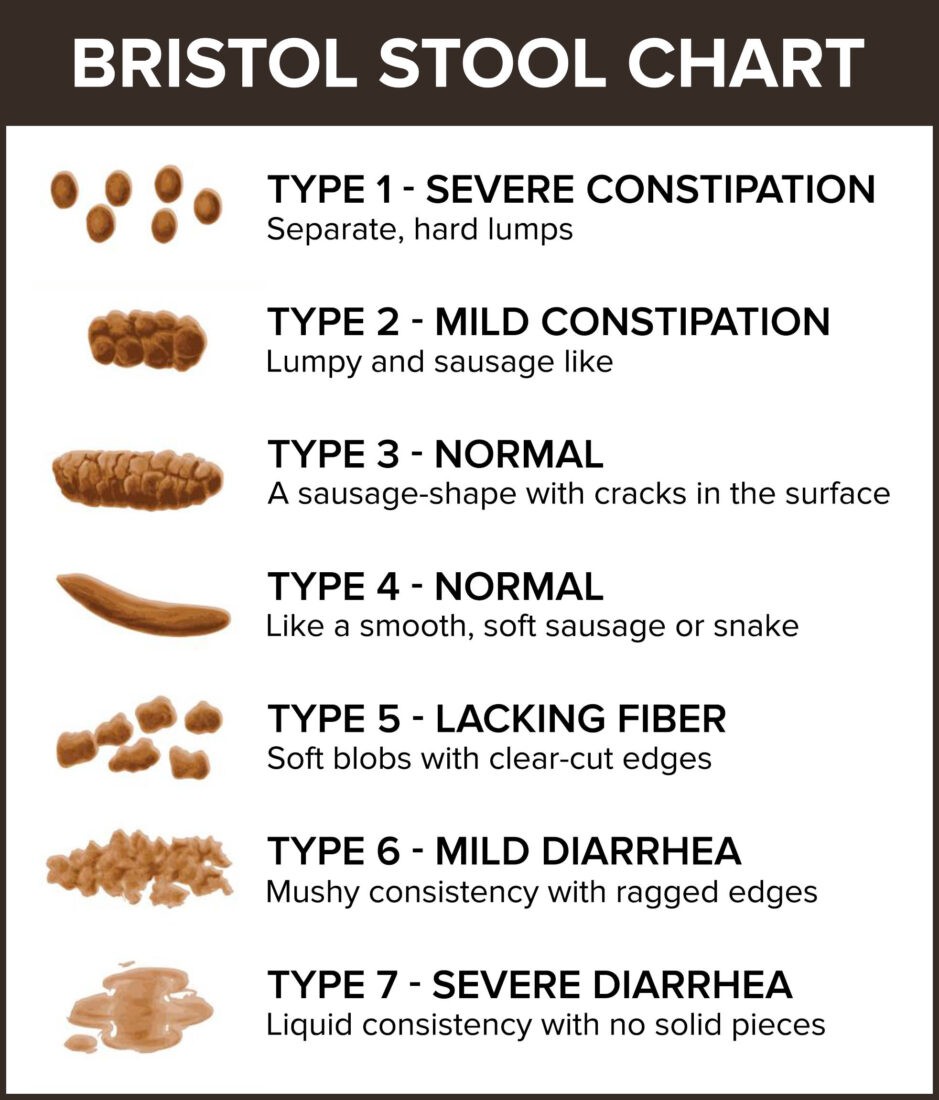
The Appearance of the Stool
Look at the Bristol Stool Chart below. Types one and two are obvious indicators of constipation. However, types six and seven may indicate diarrhea or a blockage caused by constipation, as mentioned above.
Toe Walking
Toe-walking may occur because constipation is so painful. Or, it may be a child’s way to withhold stool. This paper on constipation states, “standing on toes, extending legs or rocking back and forth preventing anal relaxation are typical features [of constipation].”
Child is not Growing
A lack of growth may be due to malabsorption problems or a lack of appetite due to constipation. This study demonstrates how constipation has a direct effect on growth in children.
Stinky Poop
Contrary to popular opinion, poop should not smell horrible. If stool smells exceedingly awful, it may be because of an overgrowth of pathogenic bacteria, or because poop has been sitting and fermenting in the colon for far too long. Stool that moves through the intestines at the right pace should not smell unusually awful.
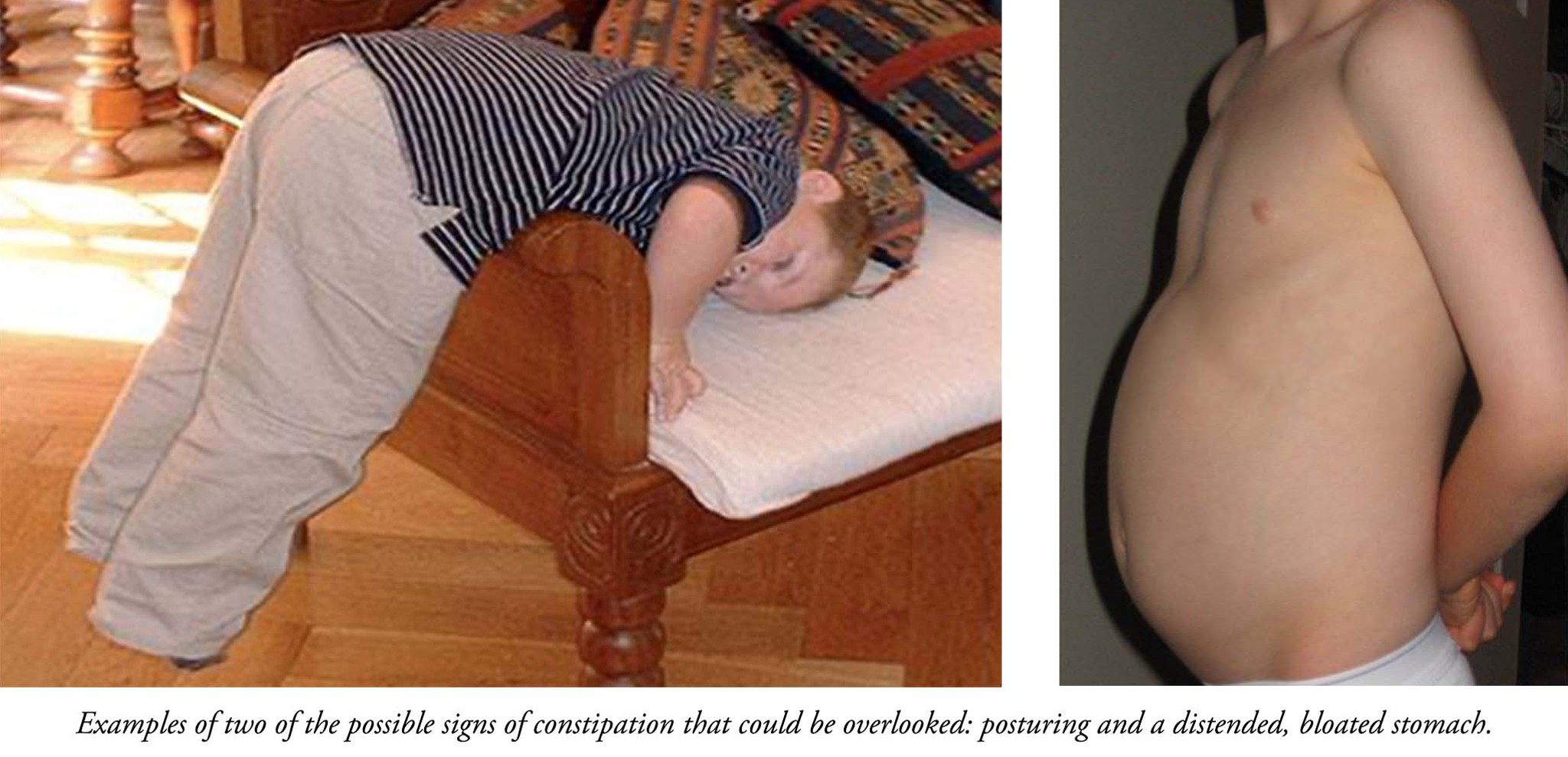
Posturing
Posturing is when a child leans over something to put pressure on their abdomen. Counter-pressure from posturing can relieve abdominal pain.
Bloated Belly
Sometimes our kids have huge, distended bellies. This may be because there is a build-up of old stool or another problem such as small intestine bacterial overgrowth (SIBO).
Streaks in Underpants and Poop Accidents
Poop accidents and streaks in underwear can be a sign that your child is not fully eliminating all the stool in their rectum. If they don’t have complete bowel movements, poop can collect in the rectum, causing it to overstretch. If your child’s rectum becomes overstretched, they may lose the urge to poop and have accidents without even knowing it.
This short video explains why constipated kids will have poop accidents and smears in their underpants.
Bed-wetting
Too much stool in the rectum doesn’t leave room for the bladder to expand, so urine accidents become more common.
Unable to Toilet-Train
When stools are unpredictable or hard-to-pass, toilet-training is going to be almost impossible. Addressing constipation needs to come first.
Toilet-Trained kids are taking too long to poop
It should not take a long time to pass stool. If it does, that is a sign of a problem.
Stool Impaction
A stool impaction is a severe bowel condition in which a hard, dry mass of poop becomes stuck in the colon or rectum. It is tremendously painful.
Symptoms of a stool impaction include:
- A distended tummy
- Night waking because of pain
- Dramatic changes in behavior
- Signs of encopresis, where soft or liquid stool bypasses the blockage, such as:
- Thin, ribbony stool
- Chronic or alternating bouts of diarrhea
- Streaks in underpants and poop accidents
- Loss of appetite
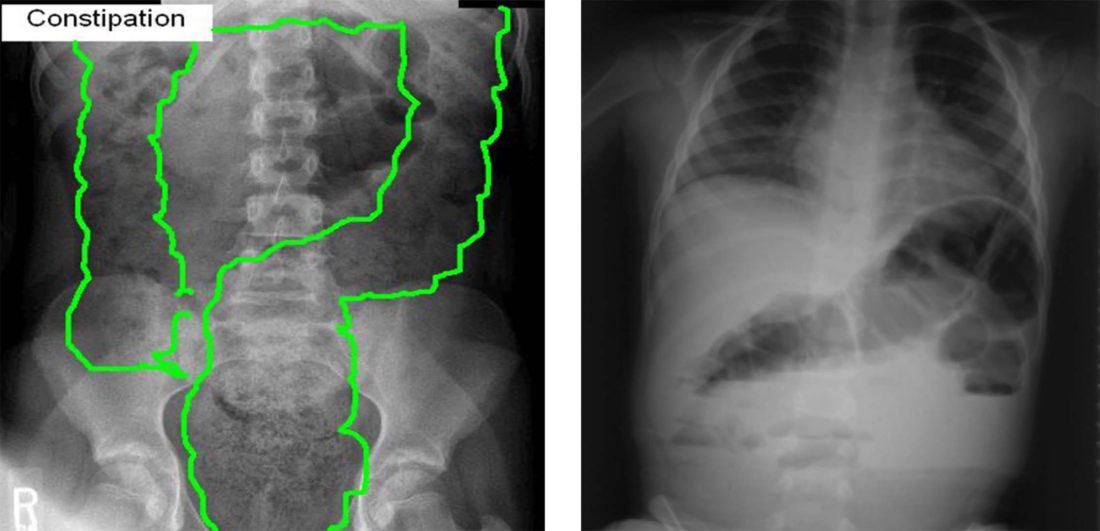
To look for a stool impaction or a large amount of stool in the colon, your child’s doctor will order an abdominal x-ray called a KUB. If an impaction is found and is large enough, it may require medical attention. If a large stool burden is found, most likely, your child’s doctor will prescribe a bowel cleanse to empty the colon and rectum of the hard poop. For information on how to do a bowel clean-out without MiraLAX, see the TACA downloadable called “Bowel Cleanse Instructions“.
Diarrhea in Autism
Frequent diarrhea that occurs once to several times a day per day is a serious medical issue. If diarrhea continues for a prolonged period of time (3-4 days), please contact your doctor immediately.
Possible Causes of Diarrhea:
- Too much:
- Fruit
- Magnesium
- Vitamin C
- Essential fatty acid (Omega 3s)
- Fiber
- Drinking bathwater that contains Epsom salts
- A reaction to food(s) or additive(s)
- Parasites such as Giardia
- Pathogenic bacterial overgrowth
- Antibiotics (that have skewed the balance of the gut flora)
- Infection such as Clostridium Difficile
- Inflammation in the intestines
- Other issues that need to be identified by a pediatric gastroenterologist
Possible Causes of Chronic Constipation and Diarrhea
Below, you will find descriptions of some of the most common causes of chronic constipation and diarrhea in autism. Familiarizing yourself with these causes will help when advocating for your child at doctor’s appointments.
Supplements and Medications
Prescribed medications and supplements commonly given to people with autism can impact the bowels. For example:
- Medications such as Risperidone, Abilify, and some prescriptions used to treat ADD/ADHD have side effects that include constipation.
- Iron, calcium, and 5-HTP are supplements that commonly cause problems with constipation.
- Your child’s doctor may suggest adding or increasing magnesium citrate or something else to keep stool soft.
- Binders such as activated charcoal can also cause constipation.
- If using, give them with plenty of water and monitor your child.
- Some probiotics, especially Saccharomyces boulardii, can cause constipation or diarrhea.
- Too much magnesium, fish oil, or vitamin C can cause loose stools.
- When starting or increasing these supplements/medications, monitor bowel movements closely.
Mitochondrial Dysfunction
Sometimes constipation is due to mitochondrial dysfunction, which is very common in kids with autism. It can slow down gut motility causing chronic constipation. Therefore, addressing mitochondrial dysfunction with a mitochondrial cocktail can be very helpful.
To learn more about Mitochondrial Dysfunction and Autism, click here.
Thyroid Dysfunction
Thyroid dysfunction is another medical condition common to autism that can cause trouble with bowel movements. For example, hypothyroidism can contribute to constipation and many other issues, including developmental delay. Whereas hyperthyroidism, less common, can contribute to diarrhea.
Food Allergies/Sensitivities
Food allergies or sensitivities could be at the root of the problem. Testing for food allergies (IgE) and food sensitivities (IgG) may be helpful.
For more information about food allergies and sensitivities, including lab testing, please read Introduction to the Gluten-Free, Casein-Free, Soy-Free Diet.
Gut Dysbiosis
Another cause of chronic constipation/diarrhea in autism is gut dysbiosis. This occurs when there is a fungal overgrowth and/or an overgrowth of bad bacteria in the gut. Gut dysbiosis is an issue that you will want to discuss with a functional medicine doctor who has knowledge and experience testing for and treating a fungal/pathogenic overgrowth in the gut. Typically, they will prescribe an anti-fungal medication or an antibiotic, which can help alleviate constipation.
A Need for Fiber
Fiber may help with constipation. But be careful: Your child must be drinking enough water with fiber supplementation, or fiber may backfire on you. Check with your doctor about brands and dosage. Favorite brands include Fibersure, ClearFiber, and TruFiber. Furthermore, always check the ingredients on the label as they change on occasion and sometimes contain wheat or soy products.
Please Note: Fiber may also be problematic if your child has mitochondrial dysfunction, SIBO, or a pathogenetic bacterial overgrowth (fiber will feed this overgrowth). Also, a fiber supplement may cause fluffy stool.
Lifestyle Tips to Help Alleviate Constipation and Diarrhea
Below you will find tried-and-true tips to help alleviate constipation and diarrhea. Some of these suggestions work for constipation, some for diarrhea, and many work for both.
- Tips that work for constipation are indicated by the letter “C” inside of a red circle.
- Tips that work for diarrhea are indicated by the letter “D” inside of a red circle.
ⒸⒹ Diet
- Eliminate gluten, dairy, soy, artificial ingredients, and limit sugar.
- Recognize foods in your child’s diet that are constipating. Milk and cheese are very constipating, and sometimes just eliminating all dairy from the diet can make a big difference.
- Bananas and nuts can also be very constipating. Monitor their intake.
- Lots of whole foods, fruits, and vegetables are helpful.
- If that doesn’t help, investigate other options like the Specific Carbohydrate Diet, Failsafe diet, or a rotation diet.
Ⓒ Healthy Fats
Healthy fats can help with constipation. Make sure your child is getting enough healthy fats in his/her diet. Some examples include:
- Fish oil, cod liver oil, coconut oil, avocado oil, almond oil, MCT oil, extra virgin olive oil, and more.
Too many fats cause loose stool, so be vigilant. And, talk to your doctor about which oils and how much of each would be suitable for your child.
ⒸⒹ Fermented Foods
Fermented foods have good live bacteria in them and can help with formed bowel movements. Start low (a teaspoon) and slowly work your way up.
Be careful with fermented food if your child is sensitive to high histamine foods.
Ⓒ Drink Water
Hydration is key! Filtered water should be the beverage of choice. It is crucial for keeping the gastrointestinal tract moving well. Ensure your child is getting plenty of water every day, even if that means sending them everywhere with a bottle of water.
Ⓒ Exercise
Exercise helps constipation in two ways. First, it decreases the time it takes food to move through the large intestine. Secondly, exercise stimulates the natural contraction of intestinal muscles.
Ⓒ A Bathroom Stool
According to this study published in the Journal of Clinical Gastroenterology, placing your feet on a bathroom stool while sitting on the toilet can help you poop. The Squatty Potty is a stool made for this purpose, but any stool will work. This video explains why squatting is far better than sitting on a toilet.
Ⓒ Abdominal Massage
Abdominal massage can be effective in treating chronic constipation by increasing the number of bowel movements, decreasing transit time, and relieving pain. Here is a video that explains how to do a bowel massage.
ⒸⒹ Raw “Green Juice”
Naturally occurring enzymes in raw fruits and vegetables will help digestion.
- Take fresh organic green fruits and veggies and puree them in the blender or juice them.
- Examples include spinach, pear, celery, or whatever is tolerated.
- Give one tablespoon of the “green juice” with each meal.
- If you use a mason jar to store the juice or smoothie in the refrigerator, it can last up to 3 days.
ⒸⒹ Fresh Squeezed Lemon in Warm Water
- Lemon makes the body more alkaline.
- It stimulates the liver and promotes bile flow, which in turn aids in digestion.
- Give this on an empty stomach, preferably first thing in the morning.
- Make sure to use a straw when drinking lemon water to protect teeth.
- This article has more information on the benefits of lemon water.
A Warning About Miralax
Often, parents are told to give their child MiraLAX to help alleviate constipation. MiraLAX is polyethylene glycol (PEG) 3350. Polyethylene is the most common form of plastic. When combined with glycol, it makes a liquid.

When a child takes MiraLAX, they are drinking plastic. If that child has a permeable GI lining, as many kids with autism do, then the plastic has the potential to cross directly into the bloodstream.
This study showed that PEG inhibited most of the fecal flora’s metabolic activities, which was demonstrated by decreases in total short-chain fatty acids, butyrate, acetate, and fecal bacteria mass. These short-chain fatty acids keep the colon healthy, and it is unknown what the outcome will be when PEG is used long-term.
Butyrate, in particular, is needed for energy metabolism. Since we already know that kids with autism have trouble producing enough energy, we don’t want to give them a product that will make it worse.
Additionally, a 2020 independent study exposed mice to polyethylene glycol (PEG), the main ingredient of MiraLax. The study showed PEG induced long-term changes in the gut microbiome, contributed to “leaky gut”, and altered immune responses. After PEG administration, the S24-7 Family of gut bacteria (within the order Bacteroidales) disappeared and was replaced entirely by outgrowth of the family Bacteroidaceae. This effect was permanent unless the S24-7 Family was replaced.
In other words, this study showed that MiraLax made poor changes to the gut microbiome that could not be undone unless the beneficial bacteria was replaced. These changes will affect the body’s immune response.
Finally, in 2021, a study titled “An Osmotic Laxative Renders Mice Susceptible to Prolonged Clostridioides difficile Colonization and Hinders Clearance” was published. It showed that mice treated with MiraLax (PEG 3350) were more prone to getting Clostridium Difficile (C Diff), a bacteria that causes diarrhea and inflammation of the colon. In addition, mice that had C Diff and were treated with Miralax were less able to clear their C Diff infection.
When choosing laxatives, it is essential to make educated decisions.
Conclusion
In summary, many children with autism suffer from painful gastrointestinal issues. Because our children experience communication and interoception challenges, parents need to watch for signs and symptoms of chronic constipation. In order to determine if your child’s bowel habits are healthy, it may be necessary to observe the frequency, texture, and amount of their bowel movements. Ideally, you are looking for stools that:
- Are formed, yet soft and easy to pass (texture)
- Are 8-10 inches long (amount)
- Occur daily (frequency)
Prolonged diarrhea and/or constipation are NOT acceptable for any child, and both require medical intervention. If these symptoms continue for more than three to four days, it is time to seek medical attention.
Above all, please contact your child’s doctor immediately if a symptom accompanies a fever; long periods of irregular bowel movements, which can lead to dehydration or other issues; extreme change in behavior; or loss of sleep or appetite for an extended period of time.






















